Journey through Cardiac Rehabilitation
This section of the academy is all about cardiac rehabilitation. The first thing I want to say is that this should not be used as a replacement for cardiac rehabilitation. It should be used as a reminder for those who have been through it or for those who are about to go through it, it can be used as a what to expect.
So in the following articles I will be going through returning home after your heart event, the time between returning home and starting cardiac rehabilitation, what is cardiac rehabilitation and then all the factors that you may be concerned about such as returning to work, travel, sex and mental health and much more.
Returning home after a heart event
It is normal to feel overwhelmed, scared and anxious after a heart event. It is a life changing experience and for many people it’s like taking a step into the unknown. But this is also an opportunity to make lifestyle changes which will stay with you forever and lead to healthier and happier life.
Recovery from your heart event can take several months, there is no need to rush your rehabilitation and there is plenty of support available to you throughout the process. This will come from your cardiac nurses, physiotherapists, pharmacists and exercise specialists.
You may have received a lot of instructions and information and now you have time to reflect you may be trying to understand how and why this happened. Maybe you are wondering what can be done to prevent this from happening again. This can be very overwhelming. I have made a few points below for what you can be doing and what to expect over the next few days and months.
Take it easy – Early on in your recovery it’s important to take things slowly and build up gradually. Getting washed and dressed each day, even when you don’t feel like it, will boost your mood. Light household activities like washing up and making hot drinks will help you start getting back into your old routines. Keeping active with short walks and walking up and down the stairs will help your recovery. It is normal to feel tired or groggy when you first start doing these activities. If you feel very unwell, contact your cardiac rehab nurse or local GP.
Medication – This may be new to you but taking your medications each day can significantly lower your chances of another cardiac event occurring. A reminder or alarm on your phone for when its time to take your medication could help you from forgetting. This is probably the most important part of your recovery and shouldn’t be neglected at all. In the learning centre you will find a whole section on cardiac medications with more information.
Managing Risk factors – This links in with the previous point about medication. Taking your medications will help manage risk factors such as high blood pressure and heart rate. Lifestyle changes can also help manage your risk factors which I will go into more detail about later on. Exercise, stopping smoking and eating a healthy diet are the best ways to manage your risk factors.
Getting support- Support from loved ones and friends can help you cope during this period, having them around for the first days can help build your confidence although you need to try and be as independent as possible.
Go to your follow up appointments – Helps your doctors keep track of your condition and recovery
*Cardiac Rehabilitation* – Last but certainly not least. Other than taking your medication this is the most important part of your recovery and brings us on to the next article.
Cardiac Rehabilitation
At this point, you may be thinking, how can cardiac rehabilitation help me? Good question. Cardiac rehab is for you if you need help:
- Understanding your condition
- Recovery from your heart event
- Making lifestyle changes and implementing them
- Psychological aspects of living with a heart condition
- Creating a support network with people in similar situations
Cardiac rehab is a programme run by a specialist team usually including cardiac nurses, an exercise specialist, physiotherapists and occupational therapists. The main purpose is to help you recover quickly and safely. The programme tends to involve:
- Education sessions, advice and talks from healthcare professionals on healthy eating, exercise, stress management and medication
- Exercise sessions
- Relaxation training
- Regular blood pressure and heart rate checks
Sessions tend to last for two hours, once or twice per week over a six to twelve-week period. A cardiac rehab nurse will be in touch to discuss when you can start. If you don’t hear from them, speak to your local GP or get in contact with your cardiac rehab nurse. You will be invited to start as soon as a place is available for you and more importantly, as soon as you feel ready to start.
It’s normal to feel nervous about starting cardiac rehab but everyone there will have been through the same emotions and your nerves will quickly be put at ease by the cardiac team. You will be invited for an initial assessment before starting the first session which will help calm your nerves and give you a chance to meet the team. Here you will discuss any questions and queries you may have, talk about the cardiac rehab process and discuss an individualised plan for you.
Common barrier to cardiac rehabilitation:
In this article I wanted to go through some of the common barriers to cardiac rehab and go through ways to overcome them. Participation rates in cardiac rehab remain surprisingly low so if you are still debating whether to go or not, hopefully the points below will help.
I’ve never exercised in my life so why would I start now? Lack of exercise could have been one of the main factors in causing your heart problems, so all the more reason to start now. You may even enjoy it! I am yet to meet anybody who hasn’t enjoyed cardiac rehabilitation.
I’m not a fan of gyms. Me neither! Luckily for you cardiac rehab gyms are tailor made to suit your needs, you will be in an environment where everybody is in the same boat. There will not be anybody wearing to much lycra (actually there might be) or oversized men grunting heavily in the weight section. Some programmes are done outside of a gym environment in town or church halls. Either way they are nothing like regular gyms.
I don’t know how to use the equipment. Perfect! You will receive one to one support in your first session to help you get to grips with the equipment and to boost your confidence and understanding.
I am fit and healthy already, I don’t think cardiac rehab is for me. I can understand this point but what I will say is you’ll be surprised. Cardiac rehab is suited to your individual needs and involves pushing people to their full potential. Experienced exercise instructors can design you a programme to help push you.
I’m scared my chest pain will return during the exercise. Whilst this is unlikely, if this does happen you could not be in a better environment for it to happen. It is normal to feel worried about this, however being in a group environment surrounded by people in a similar position and experienced staff is very reassuring.
Time between heart event and cardiac rehabilitation.
This is known as phase II of cardiac rehabilitation. Whilst there is plenty of information out there about starting cardiac rehabilitation, there is not as much information about the time between leaving hospital and starting cardiac rehabilitation. The aim of this phase is to make a smooth transition back home after leaving hospital and to start becoming stronger and more active. You will have been given a home exercise program to start, consisting of some very light exercises such as walking or stationary cycling. This will progress throughout the weeks you are at home. Your cardiac nurses will stay in touch for any questions or queries you have.
You may have already spoken to the cardiac nurses in hospital about starting your cardiac rehabilitation programme. If not, you will receive a letter or phone call inviting you to a pre rehab assessment appointment. This gives you a chance to meet the exercise specialist and speak with your cardiac nurses about how you have been getting on and discuss starting cardiac rehabilitation. You will complete a shuttle walk test which involves walking between cones which are 10 metres apart, this is to assess your exercise capacity. This may also be done at the end of your cardiac rehabilitation programme so you can see the progress you have made. Which is always very rewarding. After this you will be able to discuss starting your cardiac rehabilitation programme.
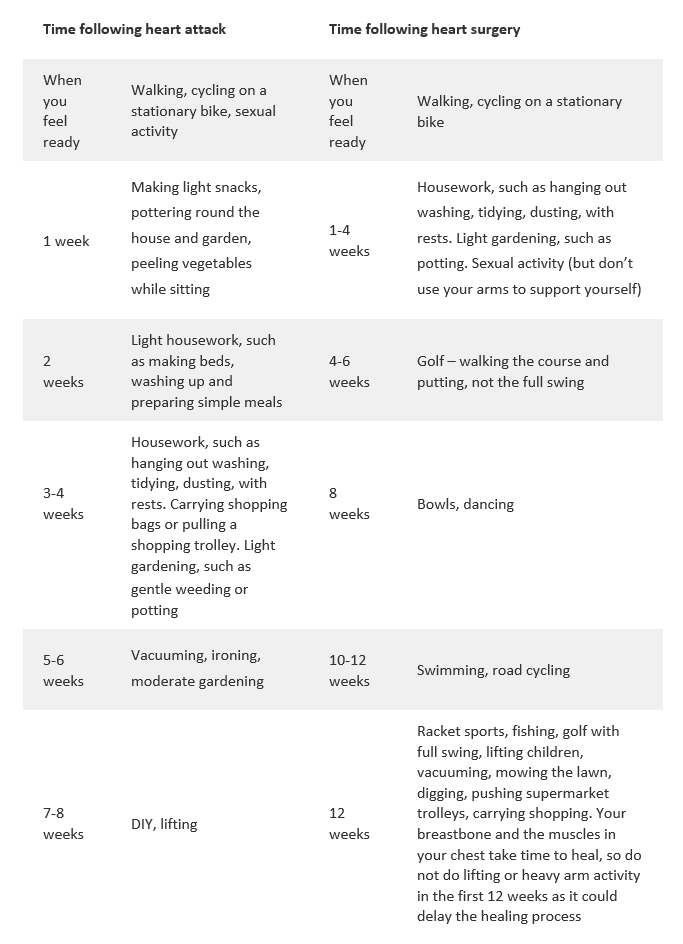
The British Heart Foundation have provided a recovery timeline, this will not be the same for everyone but it is a good guideline to follow.
Mental Health
It is common for people to be worried about their future after just being diagnosed with a heart condition. These feelings should improve as you start coming to terms with your condition. Anxiety, worry and fear are all normal responses to a life changing heart attack or heart surgery. But if these feelings don’t go away it is important to get help. It’s estimated that one in four people in the UK experience a mental health condition in their lifetime. So, this is not an uncommon thing and you are not alone with this. If you are worried about your mental health there are plenty of people you can speak to, ranging from your family and friends to your GP who will be able to tell you more about the support and medication available to help you.
Anxiety and depression can send you into a cycle of unhealthy habits including a bad diet, not exercising and using smoking or alcohol to relax. It is good to understand that these are only short-term fixes which can also make you feel worse in the long term and will also affect the condition of your heart. If you are finding there are more bad days than good, it might be time to speak to someone about it. Even speaking with a family member will help you realise you are not alone with this. There is lots of help and advice available to you and the first step is acknowledging the problem.
Striving towards a healthier lifestyle can help your body and mind. There is plenty of research out there showing that exercise helps improve your mood. Exercise releases endorphins which are also known as happy hormones which improve mood. Even going for a short walk can help take your mind off things and help you feel better. Exercising with family or friends is another great way to start.
Eating a healthy balanced diet will also help. Mental health problems can affect your appetite, so it is advised you get into a routine with your meals and it is especially important to have breakfast. Research shows that people who eat breakfast regularly are more likely to keep a healthy weight than those who do not. I believe this is because if you do not eat breakfast you become hungrier later in the day or evening which is when we begin to snack. However, you do not have to cut out your favourite foods, from time to time it’s important for your mental health to treat yourself. Planning ahead can also help, ensuring you have all the foods you need and even batch cooking and freezing meals so on the days you don’t feel like cooking there is already a meal there for you. I know these sound like quite straight forward things but they are very effective.
Driving
After a heart attack it is common for people to start driving again after just one week. This is if you do not have any other conditions or complications that would prohibit you from driving. In more severe cases you may have to stop driving for up to one month. This is of course dependent upon your condition and your cardiac rehabilitation team or doctor will be able to give you a more accurate estimation of how long to wait.
If you are a car or motorcycle driver and you have had a heart attack you do not need to inform the DVLA. However, if you drive a large goods vehicle or passenger carrying vehicle you have to tell the DVLA. You will have your license suspended for a minimum of 6 weeks until you have recovered and you will have to pass a basic health and fitness test before regaining your license. Also, they will check that you do not have any other conditions which would disqualify you from driving. Basically, the best advice I can give here is to ask your cardiac rehab team.
Travelling with a heart condition
The British heart foundation recommend that people with heart or circulatory conditions are able to go on holiday as long as they are in a stable, well controlled condition and you feel well enough to go. It is advised you check with your GP first.
In terms of how soon you can travel after a heart event this depends on your hearts condition and type of heart event. For those who have had a heart attack, it is primarily dependent on how likely you are to have another heart attack. The British Cardiovascular society categorise you as low risk if this is your first heart attack, you are under 65, have no complications and you have no further treatment planned. If you fall into all of these categories, you may be able to fly as early as 3 days after if you so wish too. Although I would advise waiting atleast 7-10 days. The UK Civil Aviation Authority recommend people at low risk fly 7 to 10 days after a heart attack. To get a better interpretation with regards to your specific condition I would strongly advise checking with your GP if you plan to fly this soon after.
In comparison, if you are over 65, have had a heart attack in the past but have no symptoms, no other heart conditions and no further treatment planned this makes you medium risk and so can fly 10 days after your heart attack. However, if you have further treatment planned or show signs or symptoms of a further heart event this makes you high risk and it is suggested you wait to be in a more stable condition before you fly. In any case I would recommend speaking with your GP before you fly.
For those of you with heart failure, the National Institute for Health and Care Excellence (NICE) recommend that most people with heart failure can travel by plane. You may find during the flight that your legs and ankles begin to swell, be aware this is normal. If you have severe heart failure breathing can become more difficult so once again it is suggested you consult your GP.
It is important to ensure you take enough medication to last throughout the time you are away, if flying you can take essential medication in your hand luggage including liquids creams and gels as long as you have a letter from your doctor explaining what they’re for and get approval from the airline before you travel. Consider packing some extra medication in your hold luggage just in case of emergencies. Although, I am sure you already thought of this!
It is a good idea to check the medication restrictions in the country you are flying too. GOV.UK has a full list of foreign embassies in the UK where you can contact the embassy for the country you are visiting. It is advised you discuss with your GP before going to countries with extreme temperatures or high altitudes. These climates and altitudes can place added strain on your heart. And finally, if you have an ICD or pacemaker, scanning devices and metal detectors at airport security should not cause a problem and won’t be set off. You can take your device identification card and inform the airport staff and ask for a hand search instead if you so wish.
That brings us to the end of travelling with a heart condition.
Sex after a heart event
Now, I wanted to include this article as it is a very underappreciated subject and can be embarrassing and difficult for people to talk about. However, that does not eliminate the importance of this subject.
Returning to sex after a heart event can be difficult for people. Now, whilst sex doesn’t count as part of your exercise for the day, which I think is slightly questionable, your heart rate will increase and your heart will be working harder which for some people can be worrying. It is important to note that having sex does not put you at more risk of having another heart event than any other form of activity. The British Heart Foundation recommend you’re able to start having sex again once you feel well enough too, roughly 4 to 6 weeks after your event. This topic should be covered during cardiac rehabilitation. If not, talking to the cardiac team or local GP is a good place to start.
It’s common for people to ignore the problem as its slightly embarrassing to talk about. I want to reiterate the point here that you’re not alone in this and there are plenty of people going through a similar thing. To prove this, the British Heart Foundation conducted a sex survey. More than 2400 people with heart and circulatory disease took part. Nearly one in five people found sex impossible. The key message is, you’re not alone. In the majority of cases, sexual problems are not caused by the heart condition but instead by the worry and anxiety relating to it. It is all too common for men to be too embarrassed to ask/ answer questions relating to their sex life but this is an extremely important part of yours and your partners relationship and shouldn’t be left unspoken. The first step here is acknowledging the problem and then beginning to seek help. Speaking to a friend, family member, GP or even reading this article or searching on google for help is the next step. Being open and honest and accepting the situation and doing something about it far outweighs ignoring it.
My next point is about erectile dysfunction (ED) which is a common problem for men with heart conditions. This is normally due to anxiety, but can also be a result of heart medications such as beta blockers. It’s very important to speak with your GP if you are experiencing problems. While your heart medication is first priority there are other medications that help with ED that you and your doctor can discuss. Neither your doctor nor you should think too little of the importance of a healthy sex life. There are treatments available to help you and your partner. Currently in the UK all treatments for ED can be taken by men with heart disease and high blood pressure but they must be prescribed by your doctor.
I found an inspiring story on the British heart foundation website called Roger’s story. It’s all about the sexual problems he experienced after a heart event and for anyone in a similar situation this may be able to help you.
Roger’s story https://www.bhf.org.uk/informationsupport/heart-matters-magazine/wellbeing/sex-when-you-have-a-heart-condition/roger-fox
Returning to work
Getting back to work is beneficial to your mental and physical recovery. It’s normal, for most, to want to get back to work as quickly as possible after a heart event, but important not to rush it. It is also common to be concerned about returning, many people think they will not be able to work again after a heart event. This is rarely the case.
How quickly you return to work will depend on your condition, the state of your heart and the type of work you do. Typically, jobs that require heavy manual tasks require a longer recovery period before returning when compared to lighter duty jobs such as office admin. Your cardiac team will be able to give you a good prediction of how long this is likely to be.
It could be beneficial to take some time to think about how your heart condition can now affect you in the workplace. You can consult your cardiac team, GP or employer to discuss this. Starting off with less hours and building back up to full time after a few weeks might help. Even starting off by working at home could be an option. Attending cardiac rehabilitation, not switching jobs, gradually returning to work and keeping in contact with your GP were highlighted as the best ways for a successful return to the workplace.
The Equality Act 2010 states ‘employers have a duty to make reasonable adjustments to prevent an employee being at a disadvantage because of their health condition’. It is worth speaking with your employer about this.
Now may be the time to ask yourself am I ready to go back?
A study I found reported that between 67% and 93% of patients return to work in two to three months. After one year, 25% quit. The study went on to say psychological factors play a key role in this decision. Lack of confidence, depression and anxiety are all factors that come into play when returning to work which reiterates my point not to rush back, really take some time to think about the best way for you to return.